Clinical Case 115: Pneumothorax puzzle
This case was interesting for a number of reasons. It starts with a 50 year old lady whom has been assaulted. She says she was kicked in the head and chest. In ED she is looking sore but stable – and it was felt that she had enough mechanism to warrant a CT of her head and neck. On the neck CT it was noted that she had some surgical emphysema on the lower slices – so she stayed in the tube for a chest scan too! Here it is:
Now – I know what you are all thinking… that is a CT image that should never had been captured! We have all heard the addage that you should always pick a tension clinically and never need to image it… but… the honest truth is that we just are not that good at picking pneumothorax clinically. As you know I am an ultraosund tragic – and I believe we can certainly pick em with a quick chest probe. However, relying on clinical exam is just not, well, reliable.
In recent years one error that I have seen creeping into my practice is the tendency to “fast-track” trauma patients to imaging where appropriate without completing a fully thorough secondary survey. There are a lot of reasons (? excuses) for this:
– trying to get the imaging done in office hours,
– trying to get patients out of collars ASAP,
– relying on second-hand info via handover which may be innaccurate….
– search satificing. Stopping at one major injury!
So my “lesson learned” here is to be systematic and make sure that you are imaging everything that needs imaging and that you have excluded the big “killers” before settling for a CT.
OK – back to the case.
A chest tube was placed and the pneumothorax decompressed. Post ICC films showed a well expanded lung. Our patient was admitted to the ward. Lets jump to the next day…..
Our patient starts to deteriorate. She is becoming more hypoxic with tachypnoea. What is going on?
Well there is a few possibilities. The chief concern was that the tube was occluded / dislodged resulting in reaccumulation of the Ptx. So another CXR was performed…
Take a few minutes to look at this CXR. It was reported by the Radiologist as “recurrence of pneumothorax on the right, with overlying subcutaneous emphysema mimicking lung markings.”
OK – let’s hear your comments. I you were at #SMACCUS last week then you will have a distinct advantage over the other readers as this case was put up in a session there and discussed.
There are so many potential errors that we can make in even the simplest of cases. Trauma is a complex scenario with information overload, serious sequelae and time critical decisions to be made. So over the next few months I am hoping got run with a theme of “common errors and their mitigation”. Hoping to have a few special guests on to help show how we can avoid the pitfalls and do better on the floor.
Casey

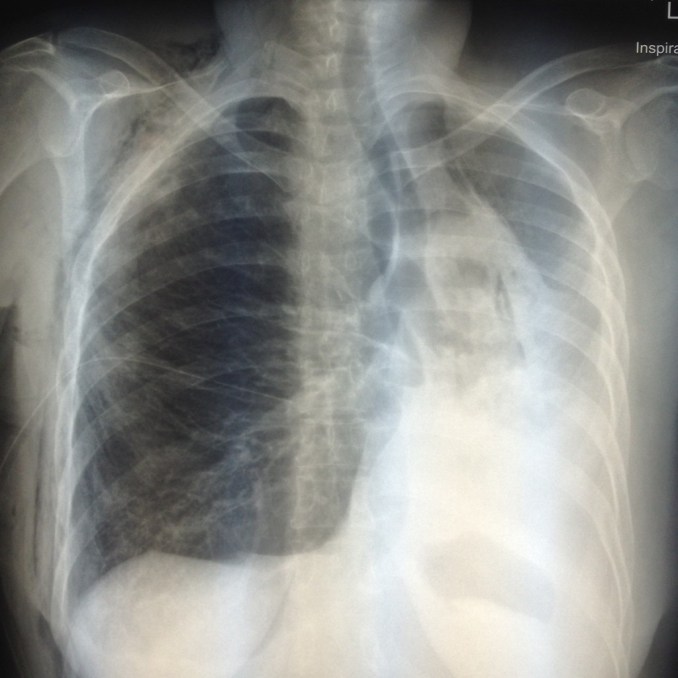



Looks like they need good pulm toilet-L looks collapsed and R look pulled to left without PTX that I can see?
tension P. Needle. Or fiddle with the tube you have in
The options are tension on the right and haemopneumothorax with collapse on the left. Loss of the costophrenic angle on the left suggests that some of the latter is likely. Is the tube swinging/bubbling? If not, take it out and fingersweep it to alleviate any potential tension (under aseptic conditions). Then ultrasound or CT the other side to see what is going on there, and/or put in a tube on the other side.
Not convinced about the “mimicking lung markings” bit. I think it is more likely to be lung collapse on the left.
Check the tube, listen to the chest, but obviously ultrasound to differentiate!
Tension ptx on R. Do needle decompression.
Get out the ultrasound probe and differentiate the consolidated lung from the pneumothorax
No X-ray? No problem!
(see, I learned something in Chicago)
the chest tube would have been enough to address the pneumothorax. its more than poking a needle. the shift of the mediastinum to the left can result to atelectasis of the left lung.