Clinical Case 086: from Hell’s heart I stab at thee
Today’s case is a tough one. This is not a happy story, but can you make it end well?
So lets lay it out and narrow it down to a few key decision points.
The patient is a 35 year old woman with a long history of schizophrenia – she has suffered with persecutory, paranoid delusions for many years. She also has a tendency to use alcohol to “self-medicate”. She is closely monitored by a community mental health team and has been managed under a community-treatment order for the last few years.
Recently she has been under a lot of stress and she has increased her alcohol use. You have seen her in ED a few times with self-inflicted injuries resulting from delusional actions.
Tonight she has been brought in by ambulance after another delusional, self-inflicted injury….
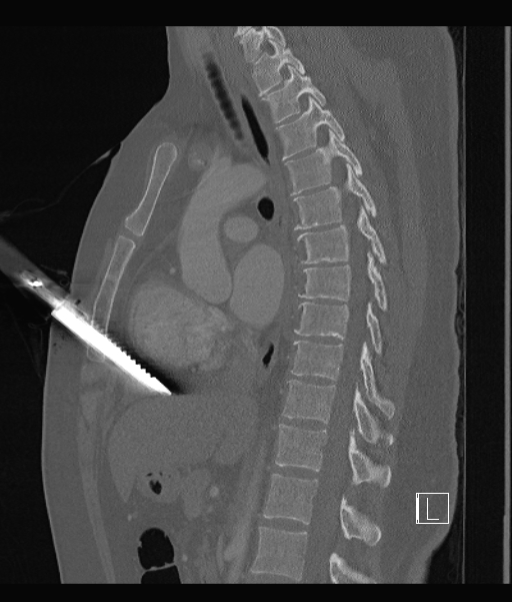
Our patient has taken a long blade and hammered it into her sternum using a heavy torch. This happened at least 2 hours ago. On arrival tot the ED her obs are remarkably normal.
Apart from a bit of blood on her clothing there is little else to find other than a knife handle protruding from her anterior chest.
As you are assessing her she has a transient dip in her BP – down from 110/80 to 85/70. This recovers without any intervention on your part.
So she gets some big IVCs, a cross match is sent, and the cardio-thoracic Reg is paged to attend ASAP.
A quick FAST / ECHO show no fee fluid, no pneumothorax, and no pericardial effusion of any volume [no tamponade effect seen either] But….. a spot troponin comes back at 0.18 – so must have some myocardial injury?
When the Surgical team arrives there is a case conference in the hallway….
They are keen to pull the blade in ED! This seems like a bad idea… after a bit of back and forth a CT is ordered
Lets assume we are in a tertiary ED with all the usual resources – ICU, cardiac theatre, trauma surgeons etc….
There was a similar case presented on Life in the Fast Lane a few months ago which you should check out for reference. There is a great “what would Weingart Do?” session around this case.
Here are a my questions for this scenario:
Q1: The super keen CT Reg is reassured by your limited bedside ECHO, and the CT appears to show no cardiac injury. He wants to give a bit of sedation and pull it out in ED – no point in bothering the nice Anaesthetic team…. what do you say to him?
Q2: Imagine you are the Anaesthetic Reg called to do a pre-op assessment for this lady. What is your basic plan to prepare for this case?
Q3: NOW, just as you are “discussing” the management paln with the CT Reg – the nurse rudely interrupts you to say: shes just gone unconscious and has no palpable pulse! Ah, bugger. What to do now? This is one of those scenarios that Cliff Reid bangs on about – you need to have a premeditated plan. What is yours? What kit do you need? Do you know where it is in your department?
Q4: Whose famous last words are included in the title of this post?
OK gang. First in best answer – you know the drill
Cover yourself in Broome Docs glory and get your answers in. Love and respect are your rewards.
Oh, and keep you eyes open for the brilliant FOAMed goodness that you can now get as the SMACC 2013 lectures are released on iTunes and the various super blogs. There will be a lecture from Dr Scott Weingart on “Just Crack the Chest” in the near future – I will link back to this post when it is available.
Here is Scott on ED thoracotomy in NYC last year. It is a biggish video so you will need a decent connection.
Cliff Reid’s “Making Things Happen” lecture was awesome – heres the link, then you will know what a ‘chicken bomb’ is! You can learn how to get control in chaotic clinical situations.
And now a week later – I have caught up with my Rural Doc Posse – Dr Tim L and Dr Minh L. WE recorded a 30 minute discussion on how we would approach this tricky case if it happened in a remote / rural hospital. Here is the PODCAST with the lads.
Casey

Q1) No. Must be done in OR with full preparation for thoractomy/sternotomy. Major point is ECG changes and transient drop in BP. Many reasons for this… could’ve picked off a coronary vessel, myocardial injury, small amount of blood may not be seen on echo…
Q2) this is an emergency situation and I would go and assess this pt right away. I would prepare the OR for double setup, and would prefer to remove knife with pt asleep to prevent movement during removal, and also have a secured airway in case of catastrophe. Blood should be cross matched and readily available in the fridge. If I were really worried, would want if prechecked and in the room. Would transport of up to OR without tubing in ED.
Q3) quickly assess ABCs and confirm pulselessness. She may have developed tamponade or arrested from myocardial/coronary injury. Either way, would perform thoracotomy and see if pericardium is tense. If tense, open pericardium and look for source of bleeding. Have foley available to tamponade ventricular tear if present.
Q4) Macbeth?
What Taylor said…except for Macbeth, that ain’t Shakespeare
I looked it up afterward… feel like an idiot! But to be fair, never read that book.
KHAAAAAAAAAAAAN!
(yes, I know, not the original source but still…)
Great case- I agree with what Taylor said. Pulling this blade out in the ED would be a clean kill- the CT registrar should get a smack up topside his head.
Curious to know- if you have CT surgery- if pt remained stable- would they look to put the patient on ECMO or bypass prior to pulling it or just expose everything with a thoracotomy and be prepared if the hole started pumping?
Usually not, because going on bypass/ECMO requires full anticoagulation (like >30,000 U Heparin) and could make bleeding worse. Also, major risk to putting someone on ECMO/CPB when there *may* not be a structural injury to the heart.
I think a TEE once the patient is intubated to look more closely would be warranted.
I concur with all – (the blade gets pulled out in ED over my dead body. Resulting in 2 corpses, I would imagine) – except the quote. This is Moby Dick is it not?? ( a recent read to children – ‘ugh. Too many ‘thee’s’ )
We have a winner!
First non-Trek related answer!
Do you ever feel like Ahab at the end of a shift?
C
The CT reg is a muppet and needs to be educated
The quote is from Moby Dick – and also STar Trek 2 – Wrath of Khan
I was surprised that this scenario was laid out in a tertiary hospital…lets spice it up a little – how would you deal with this scenario in a rural hospital in Australia?
Your team is RN-EN, orderly, GP on call and back up theatre team comprimisng 4 RNs and GP-anaes colleague
Retrieval to a tertiary centre would take 3-4 hrs to organise
She’s dropped her BP. Crack to cure?
Not unrealistic – after all, critical illness does not respect geography. So how would you manage this as a bush doc?
Ok Tim
We will discuss. Tough call, logistics may change management
Lots of variables – one needs to know team, environment and resources to make the call
Hangout? You are the “local expert”
C
Sure. Lets make it threeway…anyone else up?
Nurse would have pulled out because it was in the way of the ecg dots!
But seriously… on KI,
GET HELP
Remember ABC…
Call Tim and hopefully he isn’t teaching EMST
Call Medstar
Two big intravenous lines in.
Pray the helicopter gets here soon
Don’t let anyone touch the knife, including the patient so maybe she’ll need sedation.
Pray the helicopter gets here soon
No USS that works well enough for me to see anything but a fetal heart. Just a big knife handle hanging out of a chest. Moving in synchrony with her heart beat…..
Pray the helicopter gets here soon
AP and lateral with the mobile xray.
Pray the helicopter gets here soon
Left sided chest drain – I guess lots of blood coming out is bad (oxytocin doesn’t help this one I presume)
Pray the helicopter gets here soon
Blood pressure crashes….would I be brave enough open up her chest. Do I know how?
Pray the helicopter gets here soon
Useful snippets
http://aucklandhems.com/2012/11/13/pre-hospital-thoracotomy/
– some vidoes of the procedures
http://www.uk-hems.co.uk/Thoracotomy.pdf
– no pictures
http://emj.bmj.com/content/22/1/22.full.pdf+html
How to do it!
I do like the comment in this paper…..”Opportunity for practice is extremely limited. The first time the procedure is performed it is likely to be for real”
Now I have an idea but that could be a bad thing……
Need I say Pray the helicopter gets here soon
I’d love to hang out, but I might just sit right down and write myself a letter instead. After all, the pen is mightier than the sword. Or than the letter opener. Goods case Casey!
Sorry Casey, but the introduction picture you used for this blog is nearly identical to Bon Jovi’s trademark. Well done in your taste
Dave – it is all about the love. Probably a lot of confused BJ fans out there.
Sent you some links for the presentation next week
C
The quote is from the book Moby Dick. The quote is said by Captain Ahab.
Great case Casey. I like Tim have been thinking about I would (and could!) do in a rural hospital setting with limited staff and imaging. My approach
1) DRABCs
Danger is a big one here, if you have a schizophrenic pt who has been delusional enough to ram a steak knife into their chest, who knows what else they might do. I would call for all nursing staff (2-3 in our country hosptial) and perhaps even the police.
Put in your two big lines as you’ve said and run IV fluids/2 units of blood that is on hand. I could manage an arterial line. Sedation if she’s thrashing around potentially making the injury worse. I could probably do a chest drain after needle decompression if pneumothorax is the issue.
2) Call for real help
Retrieval team via phone or video conference. Would be wanting the team to get in the plane quick smart but also to advise about what to do in the meantime. Im not actually sure what else I could do apart from managing ABCs, and waiting for help. Would there be scope for pulling the knife in a remote country location? Cracking the chest is out of the question.
Interested to see any other thoughts for remote practice…
One thought I had whilst listening to the three twitterati (more neologisms) was how hard would it be to actually disengage that knife from the chest assuming it has been hammered through the sternum? Whereupon I recalled my boy scout leader tirade during bayonet drills – “thrust, twist, withdraw….. “If the thrust didn’t do do fatal damage, the twist and the boot to the chest to lever the cold steel out to complete the withdrawal would !